Varicose Vein Removal San Diego
Say goodbye to varicose veins with our state-of-the-art treatments in San Diego. From ClosureFast™ to VenaSeal™, our clinic offers a range of effective solutions for varicose veins with minimal discomfort and maximum success.


What is varicose vein removal?
Varicose vein removal in San Diego encompasses a range of advanced procedures designed to alleviate the discomfort and appearance of varicose veins. encompasses a range of innovative techniques, including ClosureFast™, VenaSeal™, Radiofrequency Ablation, and Varithena®. These advanced procedures provide effective relief from varicose veins while minimizing recovery times and scarring.
Free Vein Screening
If you are suffering with strange and unusual symptoms such as burning, itchy, or heavy legs, we might be able to help you.
How each varicose vein removal works
Explore our comprehensive varicose vein treatment options at our Varicose Vein Clinic in San Diego. Our services include:
Radiofrequency Ablation: A minimally invasive procedure using thermal energy to seal varicose veins.
Varithena®: An injectable foam treatment designed to address varicose veins effectively.
ClosureFast®: Utilizes radiofrequency energy for precise vein closure, reducing discomfort.
VenaSeal®: Seals veins with a medical adhesive, offering a safe and efficient solution.
Compression Stockings: Elastic stockings designed to enhance blood circulation and alleviate varicose vein symptoms.

Discover the benefits of varicose vein removal at our vein care clinic
We use modern techniques to treat varicose veins, customizing our approach to each patient. This may involve using foam or radiofrequency to collapse the damaged vein.
Custom treatment plan
Experience safe and minimally invasive treatments performed by skilled specialists.
Quick and Virtually Painless
Varicose vein treatment is minimally invasive with limited downtime, and patients can often return to work the same day.
Little to no pain
Local anesthetic ensures a comfortable varicose vein procedure
Varicose vein removal
Patients with varicose veins may experience relief from symptoms as veins disappear.
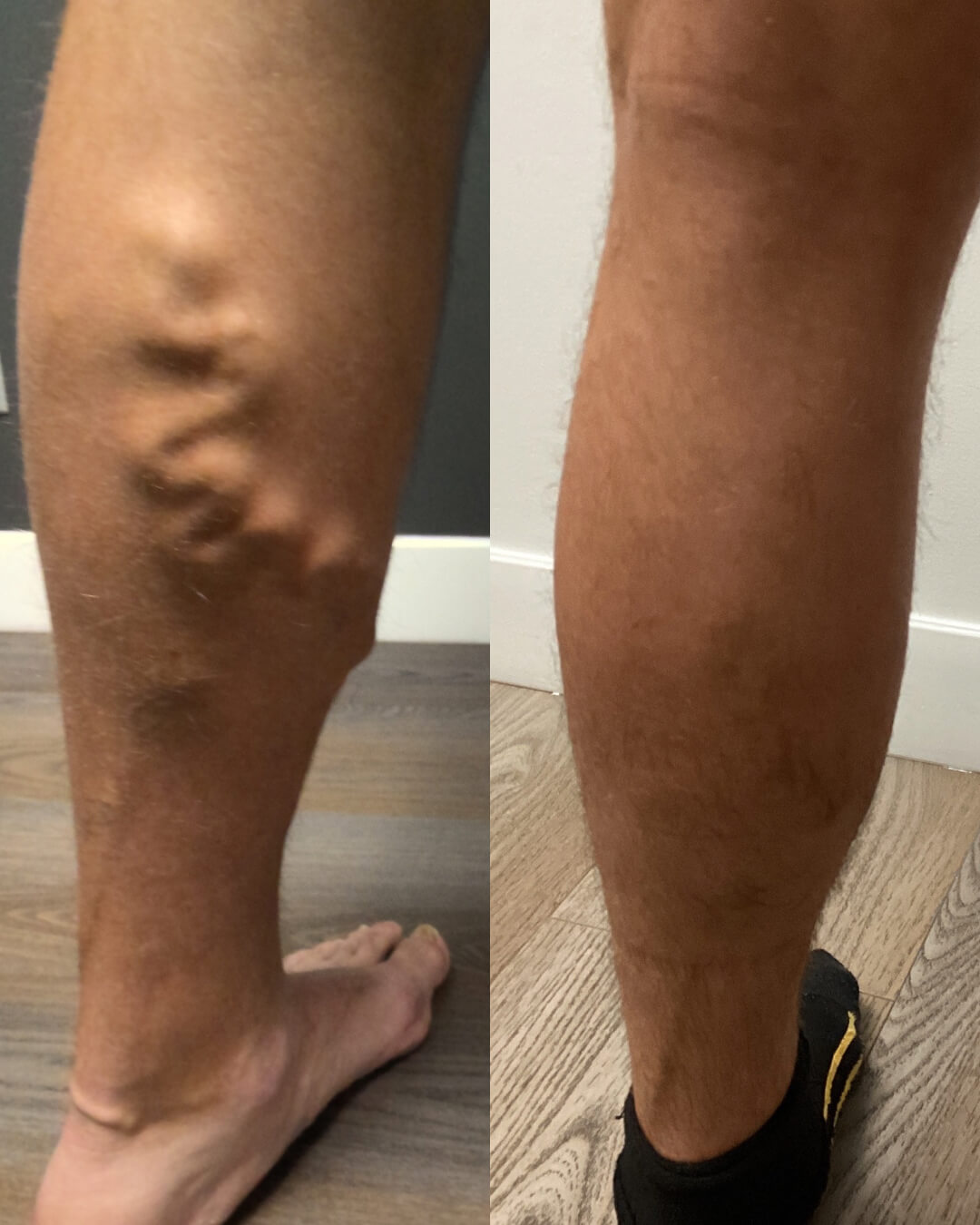
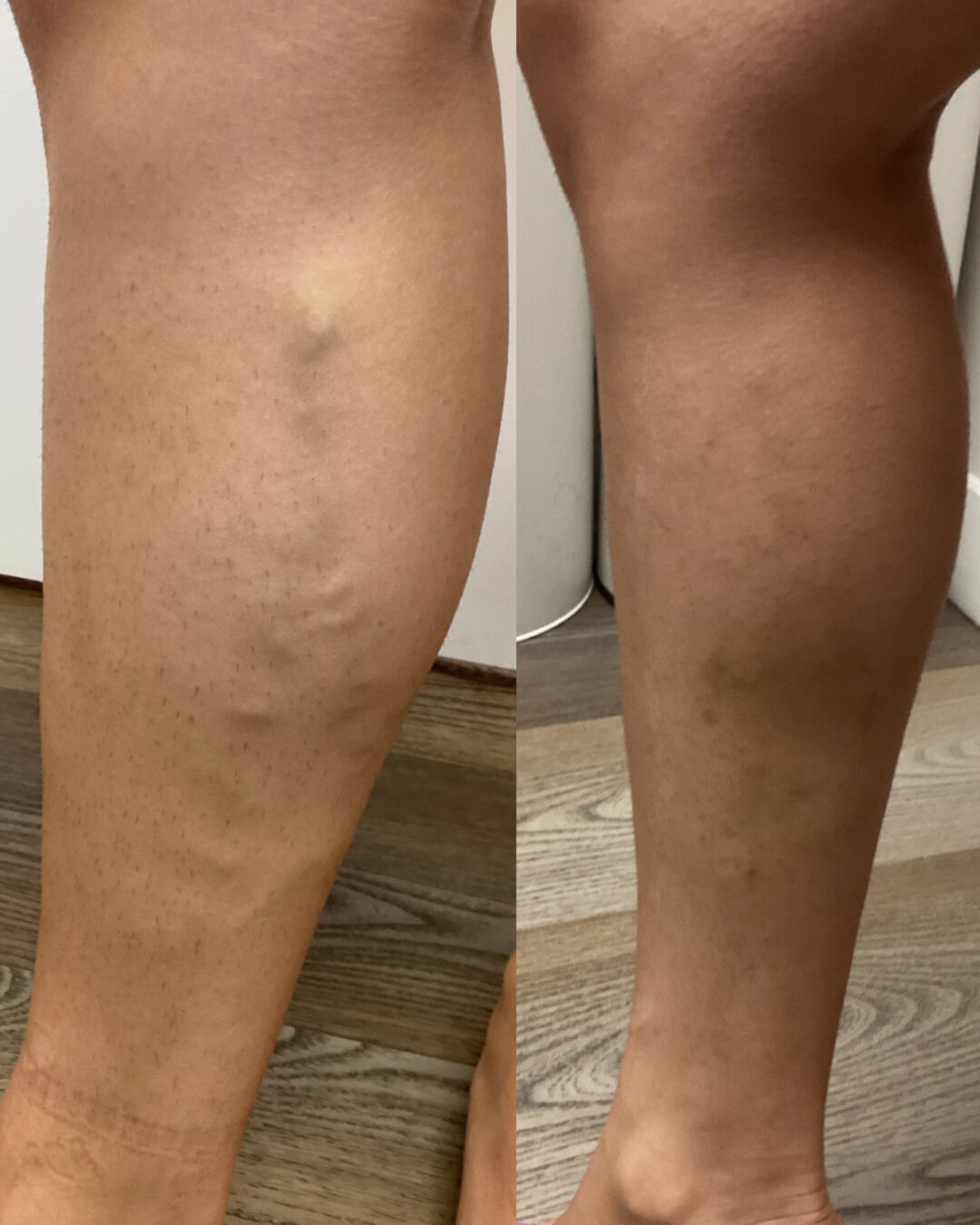
Successful before & afters
See the amazing transformations of our patients' veins!

Why is it important to treat your leg varicose veins?
Treating varicose veins on the legs is crucial to ensure your overall leg health. If left untreated, leg varicose veins can lead to various complications, including:
Pain and Discomfort: Untreated leg varicose veins can cause persistent pain, aching, and discomfort, making everyday activities more challenging.
Blood Clots (Deep Vein Thrombosis): Varicose veins can increase the risk of blood clots, which can be life-threatening if they travel to vital organs.
Burst and Bleeding: Over time, untreated varicose veins may become more fragile, potentially leading to burst veins and significant bleeding.
Proven Success: A track record of happy patients and outstanding results.
Meet our varicose vein removal San Diego doctor
We pride ourselves on merging years of hard-earned experience with the latest advancements in vein care. Every patient benefits from our deep-rooted knowledge and the innovative varicose vein treatment technology.

- iThriveVeins Patient
Varicose Vein Treatment Options
We offer a variety of treatment options for varicose veins. Contact us today to find out which is best for you.

Get your free vein screening
Our medical professionals will speak with you over the phone to gather information about your symptoms.
Free Vein ScreeningFAQs
Have questions about Varicose Vein Treatment in San Diego? Check our frequently asked questions to learn more about what to expect at our San Diego varicose vein treatment center.
Varicose vein treatment costs can vary depending on the specific procedure and your individual needs. It's best to schedule a consultation with our experts for a personalized assessment and cost estimate.
Insurance coverage for varicose vein treatment depends on your provider and the medical necessity of the procedure. Our team can help you navigate insurance matters and determine if your treatment qualifies for coverage.
Yes, several minimally invasive treatments can effectively eliminate varicose veins without the need for surgery. Our specialists will recommend the most suitable option for your condition.
To potentially have insurance cover varicose vein removal, you'll typically need a medical diagnosis indicating that the treatment is medically necessary. Our team can assist you in the insurance approval process.
The most effective treatment for varicose veins varies from person to person. It depends on the type and severity of your condition. Our experts will assess your situation and recommend the best treatment option for you.
Minimally invasive varicose vein removal procedures are designed to minimize discomfort. Most patients report only mild discomfort or pain, which is easily manageable with local anesthesia and post-treatment care.
The quickest way to get rid of varicose veins is through minimally invasive procedures like radiofrequency ablation or VenaSeal™, which typically have shorter recovery times compared to traditional surgical methods. However, the choice of treatment should prioritize your specific needs and health.
See what patients are saying
Ready to improve your vein health?
Starting your journey towards healthier, more comfortable legs is just a click away. Fill out your details, and our team will get back to you.
La Jolla/UTC
National City
Our Locations
Visit our convenient locations for personalized vein treatments.



































.jpg)


